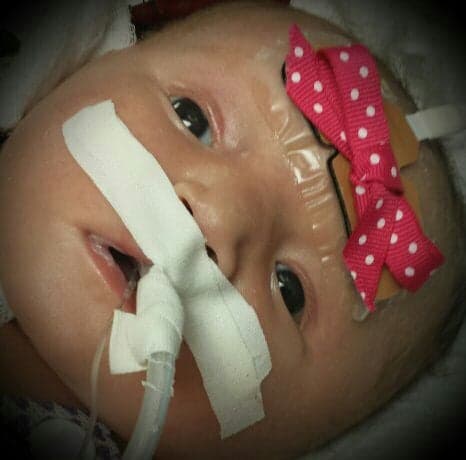
October is Pregnancy & Infant Loss Awareness month. Unfortunately, many of our heart families walk this impossible road. Help-A-Heart wanted to share the story of one of our heart angel families this month to help raise awareness. Thank you to Nate & Emily Forsythe for writing & sharing the story of their precious daughter, Kennedy Ren Forsythe. Nate & Emily are the proud parents of Kennedy & Oliver (age 1). This is Part 5 of 11.
Arterial Switch
February 17th, 2016. Surgery Day. We are in her room at six a.m. where a team is preparing her. All tiny 7 pounds, 19 inches of her. She’s crying. And hungry. They can’t feed her because of her surgery. I get to hold her while we wait to talk to the medical team. (This would be the last time I held her while she was alive – I wish it had lasted longer…) Her head is in the crook of my left arm and I’m holding her left hand with my left hand and stroking her face – forehead to her nose to her forehead to her nose. Comforted, she stops crying. And I just stare at her, taking in her tiny features, memorizing her chest, since this would be the last time I would see it without a scar.
The medical team enters. I’m not ready to let go of her, so they let me continue to hold her while they talked to us. The anesthesiologists are up first. They walk us through their process: “We’re going in through the existing lines. We’ll give her XYZ to get her to sleep, and a paralytic, and….” So many steps – I know they’re telling us because its part of their job, but it’s a lot on an already emotional day. They ask if we have any questions. (1000, but none of them really pertain to her surgery, so no.) They hand us some papers and we sign them.
This process went on for three or four groups of her surgical team.
Steps. Questions. Papers. Steps. Questions. Papers.
Dr. T- the surgeon- enters the room with his assistant. More steps. More paperwork. They walk us through The Switch. There’s a cartoon book and his assistant reviews it with us. Questions? We ask a few, confirm our phone numbers, so they can communicate with us during from the surgical room. Sign the papers.
It’s time. I have to hand her back. Nothing can prepare you for the moment when you hand over your child to a team of doctors that will cut her open and try to fix her broken heart. Nothing. They take her from me – thankfully sleeping at this point – and put her on the bed to wheel her away. They allow me to come with (thankfully). There are eight people walking down with us, each one monitoring something that is attached to her. We load into the massive elevator and head down. A nurse squeezes my shoulder – I’m certain she can see me trembling and I’m no longer trying to hold in my tears.
One floor down. The ride wasn’t long enough. We have a jaunt from the elevator to the other side of the hospital. I try to set the pace (slow, obviously), but the team is all business and are walking faster than I want them to. They stop and turn. I’m not able to go any further than this point. They allow me to kiss her cheek and squeeze her hand.
I watch them turn the corner and they’re gone.
8:02am. The walk back to the PICU was one of the longest I’d ever taken. I had just handed over my six-day-old child to operate on her heart. They scheduled the operating room for eleven hours. But it will take a long as it takes.
My family would arrive soon. We would spend the day distracting ourselves, anxiously awaiting news from the surgery.
9am. They’ve put her to sleep and administered a concoction of drugs. All is good so far.
We sit at a table in the family lounge, nervously sipping coffee.
11:09am. She’s successfully on by-pass and Dr. T has begun. They think they’ve identified a big VSD (a hole in her heart, an added complexity). The thought is that they will patch it while her chest and heart are open. They’re currently working on the switch. Everything is going well.
12:29pm. Things are moving along very well! They have finished the arterial switch and are completing the sewing of the coronary arteries. This will be the biggest chunk of the surgery, but it sounds like they will begin the process of warming her and weaning her off bypass in the next couple hours. All updates sound positive, so we relax a little bit.
We play cards. It passes the time. Hearts and Rummy, mostly.
4:38pm. I’m sitting in Kennedy’s PICU room, pumping. My sister is with me. Dr. T’s assistant comes in – weird, she usually calls. “We can’t get her off bypass.” A punch in the stomach. We are not out of the woods. She was weaned off bypass a few hours ago and did well initially. However, it seems like one of her pumping chambers is only working 50% of the time. Dr. R – the Pediatric Cardiologist – is in the OR with the surgeon and they have decided to do a cath procedure to determine where the issue is. The thought is that one of the coronary arteries may need to be repositioned. If needed, they will cool her and put her back on bypass to fix it.
I walk back to the family lounge, crying. One of the PICU moms pulls me aside and gives me a “we’ve been there and I know your pain” talk. I needed that.
I can’t focus. We play cards. Over and over and over.
10:19pm. They just completed the procedure. There were additional complexities with her little heart that were harder to fix. It appears that one of her coronary arteries spasmed and nitroglycerin had to be administered. She’ll be one something called ECMO. It’s similar to bypass – it allows her heart to relax and does the work for her. They’ll try to wean her off of it in the next 24 – 48 hours.
1:45am. She arrives back up to her room where Nate and I are anxiously waiting. She’s stable. Her chest is still open and will remain open until a day or two after she comes off ECMO. This is to ensure that if there is a problem, they can fix it quickly. Her lungs are good – the machine isn’t doing much work for her. She’s also beating her heart on her own consistently. She had a pacemaker overnight, but it is precautionary. ECMO will be in place for another day – when the heart goes through a lot of trauma, it has a hard time starting to operate as it should without assistance. To add to that, her surgery took the original main pumping chamber and turned it into the secondary pumping chamber – for the last 9 months the chamber we want to be her main pump hasn’t been working as hard as we’re asking it to.
3:00am. I go to my temporary home for a nap. I’ll be back in her room at 7am for Rounds. I don’t sleep, though. Nervously clinging to hope for a better tomorrow.